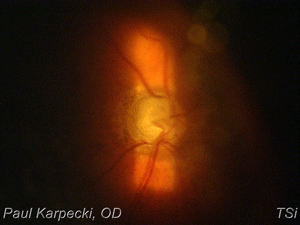
Central retinal vein occlusions occur when a thrombotic obstruction occurs in the central vein of the retina and is essentially a blockage of the portion of the circulation that drains the retina of blood. The result is a sudden complete retinal hemorrhage (bleeding) throughout the four quadrants of the retina, as well as optic nerve disc edema (swelling) and dilated, tortuous retinal veins. The major symptom you as patient will experience is a sudden complete loss of vision in one or both eyes.
Reasons for developing CRVO may involve abnormal blood flow or blood constituents (blood plasma, erythrocytes, leukocytes, and thrombocytes), atherosclerosis and vessel anomalies. Properties of blood and the vein itself act in concert to cause thrombus formation, which impedes venous blood flow from the retina.
Other associated risk factors include systemic diseases like Hypertension, Glaucoma, Diabetes mellitus, Cardiovascular disease, Anemia, Carotid artery obstruction, Hyperviscosity syndromes, Leukemia, Optic nerve drusen, Cavernous sinus fistula, Polycythemia and Vasculitis
A recent article written by Dr Paul Karpecki, OD in the Review of Optometry highlighted the high association of developing secondary Glaucoma after having a Central Retinal Vein Occlusion.
“Patients who have experienced a central retinal vein occlusion (CRVO) are at an elevated risk for the development of glaucoma. Even worse, patients with an ischemic CRVO may develop glaucoma within 90 days of initial onset.
The statistics are quite telling: Approximately 75% of patients older than 65 years of age who have had a CRVO already have or eventually will develop glaucoma. But, why is this correlation so high? Several experts have suggested that increased intraocular pressure puts stress on the retinal vein wall, which results in a loss of structural support on an already compromised nerve. Ultimately, this process results in significant retinal nerve fiber layer damage.
Another contributor is that elevated Intra Ocular Presssure (IOP)—in of itself—is a known risk factor for any form of retinal vein occlusion, and thus patients with a history of elevated IOP are more prone to a CRVO.
So, what does this mean to your practice? You should suspect that all patients with CRVO will develop glaucoma unless proven otherwise. You may want to consider treating such patients with IOP-lowering medications in questionable cases. Also, if you begin topical IOP therapy, be sure to medicate the fellow eye (assuming that no contraindications exist).”
The bottom line is that if you have any of the above mentioned risk factors you should have your eyes tested regularly irrespective if you think your eyes are good or bad. It might just save your sight one day.